Did you know that opioid-related deaths in the UK just keep climbing higher and higher?
Studies indicate that fatal overdoses involving opioids now exceed 2,000 annually in England and Wales alone, with Scotland recording some of the highest drug death rates in Europe! Recent reports have also identified emerging threats from synthetic opioids, including an estimated 64 nitazene-related fatalities.
Against this scary backdrop, naloxone has become a central harm-reduction tool across UK public health policy.
Want to know everything about naloxone and how it can literally save lives? We have covered everything for you in this guide! This article provides UK-specific information about naloxone: what it is, how it works, how UK law governs its supply, and how you can access and use it safely.
It is written within a public health framework, alongside NHS and local drug services, to support you if you’re affected by opioid use.
Naloxone is a temporary opioid antagonist used in emergencies. It is not a replacement for medical care, ongoing treatment, or rehabilitation.
999 must always be called in any suspected overdose, even if naloxone is available or has already been given.
PCP works within this UK public health and legal framework, alongside NHS and local drug services, to support you if you’re affected by opioid use through residential rehabilitation and detox services.
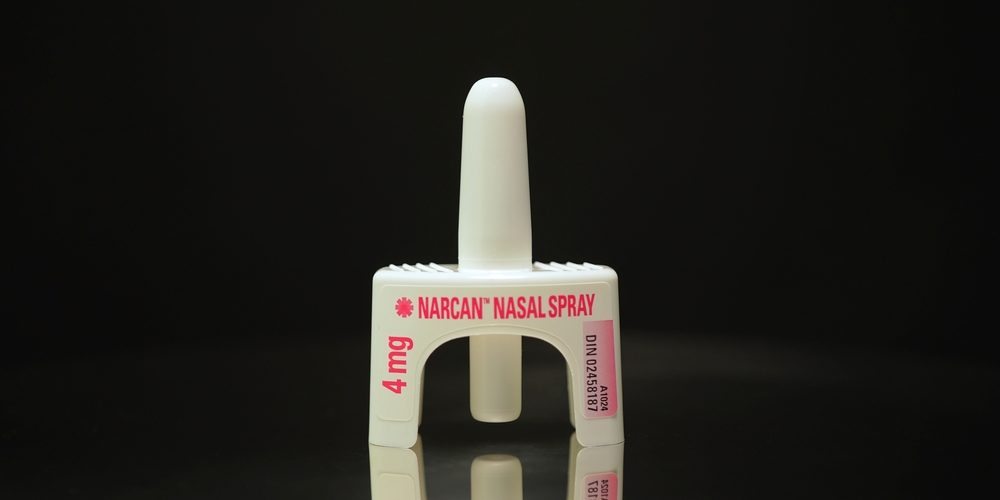
What is Naloxone?

Naloxone is an opioid receptor antagonist medication designed to temporarily reverse the life-threatening effects of an opioid overdose. It can reverse overdoses caused by heroin, methadone, morphine, oxycodone, fentanyl and other synthetic opioids.
Naloxone works by displacing opioids from their receptors, mainly in the brain and central nervous system, helping to restore breathing when respiratory depression has occurred due to opioid drugs.
● Naloxone only works on opioid overdoses; it does not reverse overdoses caused solely by non-opioid substances like benzodiazepines, alcohol, or stimulants
● It has no psychoactive effect and will not cause a “high”
● In people without opioids in their system, naloxone typically has little or no clinical effect
● Naloxone is not a treatment for opioid dependence or opioid addiction
● It is used alongside, not instead of, longer-term interventions such as detox, substitution therapy, psychosocial support and residential rehab
How Naloxone works and how long it lasts
Naloxone acts by competing with opioids at the same receptors in the brain and respiratory system.
When you administer it, naloxone blocks these receptors and temporarily prevents opioids from exerting their effects on breathing and consciousness. This is why it is classified as an opioid antagonist.
The onset of action depends on the route of administration:
● Intramuscular or subcutaneous injection: usually within 2–3 minutes
● Nasal spray: often within 1–2 minutes, depending on circulation and dose
● Intravenous injection or intravenous administration (used by medical professional teams): typically faster onset
The duration of effect is absolutely crucial for you to understand! Naloxone works for approximately 20–40 minutes, sometimes up to 60–90 minutes. However, many opioids—especially long-acting ones like methadone or extended-release preparations, or potent opioid substances like fentanyl—last much longer in the body.
This creates a significant risk of “re-sedation.” Once naloxone wears off, the person may become unconscious again and stop breathing if opioids remain active in their system. This is why multiple doses may be needed and continued monitoring is absolutely essential!
Naloxone can precipitate acute withdrawal symptoms in people who are opioid-dependent. These may include:
● Agitation and anxiety
● Sweating
● Nausea and vomiting
● Diarrhoea and stomach cramps
● Muscle aches
● Raised blood pressure and rapid heart rate
While uncomfortable, these withdrawal symptoms are outweighed by the need to restore breathing and save a life. Because of the temporary effect, emergency services must still attend and observe the person even if they seem to have recovered.
Legal status of Naloxone in the UK
Naloxone hydrochloride is classified as a prescription-only medicine (POM) under the Human Medicines Regulations 2012 (HMRs). However, specific UK legislation has been developed to allow certain services to supply naloxone without a prescription for the purpose of saving life in an emergency.
Key regulatory developments include:
● 2015 amendments: The Human Medicines (Amendment) (No. 3) Regulations 2015 enabled commissioned drug treatment services to supply naloxone without individual prescriptions or Patient Group Directions for injectable products
● 2019 update: Regulations were amended to explicitly add licensed nasal naloxone products to the list that can be supplied under these arrangements
● 2024 amendments: From 2nd December 2024, further changes to the HMRs expanded who may supply naloxone without prescription via two defined routes (often referred to as “route 1” and “route 2”), including broader community and criminal justice settings
Although supply arrangements are now more flexible under these regulations, naloxone may only be supplied and used for emergency treatment of suspected opioid overdose, within the limits set by UK law and local clinical governance.
Official guidance on these legal changes is available on gov.uk and from bodies such as the Office for Health Improvement and Disparities (OHID).
Who can supply Naloxone in the UK?
NHS and local-authority commissioned drug and alcohol treatment services across England, Scotland, Wales and Northern Ireland are the key authorised suppliers of take home naloxone.
Route 1 (named professionals and specified organisations)
Following the 2024 regulations, staff and volunteers employed or engaged by named services can supply naloxone. These include:
● Community drug and alcohol teams
● Homeless services and hostel staff
● Criminal justice services
● Custody healthcare providers
● Needle and syringe programmes
Route 2 (registration scheme)
This route allows a wider set of organisations and workers to supply take home naloxone kits once they are registered and trained, under defined conditions. This expands access while maintaining appropriate governance.
Other supply pathways
● Community pharmacies where commissioned, including pharmacies offering supervised consumption or opioid substitution therapy
● Police forces, custody suites, prisons and probation services under the expanded 2024 framework
● Primary and secondary care settings when commissioned appropriately
While authorised services can supply naloxone without an individual prescription, it remains a prescription-only medicine. Onward “wholesale” supply by organisations still requires appropriate medicines licences.
Who can Receive and Carry Naloxone?
UK law allows naloxone to be supplied to anyone for the purpose of saving life in an emergency. This includes:
● People who use opioids
● Friends and family members
● Peers and fellow residents in hostels or supported housing
● Hostel staff and outreach worker teams
● Anyone likely to witness an overdose
It is legal for anyone in the UK to administer naloxone to someone else in an emergency to save life, regardless of who it was originally supplied to.
Priority groups for take home naloxone schemes typically include:
● People using heroin or other illicit opioids
● Those receiving methadone or buprenorphine treatment
● People leaving prison or residential treatment (high-risk period)
● People who have experienced a previous non-fatal overdose
Regarding children and young people: there is no legal restriction or legal age ban on supplying naloxone if the intention is to save life. However, decisions for under-18s should follow safeguarding and paediatric clinical principles. Some nasal spray products are licensed for use from age 14 upwards—always check product-specific guidance.
Recipients of naloxone kits should not further distribute them as if they were suppliers. However, they can hand their kit to anyone present in an overdose situation to use on the person in need. Local services usually provide brief training when issuing kits so you understand when and how to use naloxone safely, and the importance of calling 999.
Forms of Naloxone Available in the UK
The main take home naloxone products available in the UK include pre-filled intramuscular injectable kits (such as Prenoxad) and licensed nasal spray formulations (such as Nyxoid). Both are designed for use by laypeople with appropriate training.
● Injectable naloxone: Pre filled syringe kits allow titrated dosing and may be more familiar to clinical staff; typically administered into the outer thigh or upper arm
● Nasal naloxone: Nasal spray devices avoid needles, which some people find easier or safer to use; a single spray is delivered into one nostril
Each kit comes with specific instructions for assembly and administration. Key practical considerations:
● Injectable kits may allow more control over dosing in small doses
● Nasal sprays require no needle handling, reducing anxiety for some users
● Ambulance services and hospital emergency departments may use other injectable preparations (including IV or IM ampoules) according to local clinical protocols
Always check the expiry date on your kit and seek a replacement from your supplier when it is close to expiring or after it has been used.
Where to get Naloxone in the UK
Availability varies by nation and local commissioning, but most areas now support take home naloxone schemes through community drug services. Access has expanded significantly since the first mainland scheme launched in south London in 2001.
Typical access points include:
● NHS or local-authority commissioned drug and alcohol services
● Needle and syringe programmes (including pharmacy-based programmes where commissioned)
● Community pharmacies involved in harm-reduction work or opioid substitution therapy
● Homeless outreach teams
● Criminal justice settings (police custody, probation, prisons)
National and regional schemes
Scotland operates a national take home naloxone programme, which expanded during COVID-19 to include “Click and Deliver” arrangements. England, Wales and Northern Ireland have similar but distinct commissioning arrangements—details differ between nations.
Some third sector, peer-led and voluntary organisations working under local agreements can also distribute naloxone and provide overdose training.
Cost
Naloxone may be provided free of charge through publicly funded services to eligible people at risk and to those likely to witness overdoses. Many services offer a free kit alongside training. If you’re seeking naloxone, you should ask your GP, community pharmacist, or local drug service how to access it in your area. Official NHS and local council websites often list naloxone providers.
How to Recognise a possible Opioid Overdose
Recognising an overdose promptly allows earlier use of naloxone and earlier calling of 999, both of which improve the person’s chances of survival. Common signs and symptoms of suspected opioid overdose include:
● Very slow or absent breathing
● Snoring or gurgling sounds (indicating airway obstruction)
● Unresponsiveness—unable to wake the person
● Blue or grey lips and fingertips
● Pinpoint pupils
● Pale or clammy skin
Overdoses often occur when opioids are mixed with other drugs such as benzodiazepines, gabapentinoids, or alcohol. They are also more common after a period of reduced tolerance, for example, following prison release, detox, or hospital admission, when drug users may return to previous doses that their body can no longer handle.
If there is any doubt, treat the situation as a suspected overdose and act quickly rather than waiting to be certain.
Training from local services usually includes practice in identifying these signs and rehearsing response steps.
How to use Naloxone in an Emergency
The following provides a general outline that applies to both injectable naloxone and nasal spray kits. Always follow the specific instructions that come with your product, and adapt based on local training.
Step 1: Check for danger and try to rouse the person
● Ensure the environment is safe
● Shout their name, shake their shoulders firmly
● Rub your knuckles on their sternum (breastbone)
Step 2: Call 999 immediately
● Report a suspected opioid overdose
● Give your location clearly
● Stay on the line if possible
Step 3: Support airway and breathing
● Place the person on their back
● Tilt their head back gently and lift their chin to open the airway
● Clear the mouth if safe to do so (only remove visible obstructions)
● Give rescue breaths if trained and able—two initial breaths, then one every 5 seconds
Step 4: Administer naloxone
● For injectable naloxone: inject into the outer thigh or upper arm muscle
● For nasal spray: insert the nozzle into one nostril and press the plunger to deliver the dose
Step 5: Monitor and repeat if needed
● If there is no response or minimal improvement after 2–3 minutes, give a second dose
● Continue monitoring breathing and responsiveness
● Further doses may be needed depending on kit instructions and local protocols—some situations require multiple doses, especially with potent opioid or long-acting substances
Step 6: Recovery position
● If the person starts breathing adequately but remains drowsy, place them in the recovery position (on their side)
● Continue to observe them closely until the ambulance arrives
● Be prepared for their condition to deteriorate again as naloxone wears off
Calling 999 and Working with Emergency Services
Calling 999 is absolutely essential in every suspected overdose—before or immediately after giving naloxone! Naloxone is not a substitute for paramedic or hospital care.
When you call 999, provide:
● The person’s condition (breathing, responsiveness)
● Suspected substances taken (if known)
● Any known medical conditions
● Your exact location
UK ambulance and emergency department staff are familiar with naloxone use and opioid reversal. Early, honest information about drug abuse or drug use helps emergency personnel treat the person more safely and effectively.
The presence of naloxone or previous drug use does not prevent emergency services from attending. The priority is preserving life. Police officers may attend alongside ambulance crews in some areas, but the focus remains on medical care.
Stay with the person until first responders arrive! Continue basic life support if necessary and follow any instructions given by the 999 call handler. When the ambulance arrives, inform paramedics that naloxone has been given, including how many doses and when.
Safety Considerations and Side Effects
Naloxone is generally considered safe when used as directed in suspected opioid overdose. However, side effects can occur, mainly related to sudden opioid withdrawal in dependent individuals.
Common withdrawal-type reactions:
● Agitation and anxiety
● Sweating
● Nausea and vomiting
● Diarrhoea and stomach cramps
● Rapid heart rate
● Raised blood pressure
● Tremor and muscle aches
Less common but more serious complications:
● Heart rhythm disturbances
● Pulmonary oedema (fluid in the lungs)
These are rare and occur more often in people with underlying cardiovascular disease or those receiving very high or repeated doses.
Despite such risks, untreated opioid overdose and continued respiratory depression carry a far higher risk of death or long-term brain injury than using naloxone.
After naloxone is given:
● Avoid giving additional non-prescribed sedative or stimulant drugs
● Provide calm reassurance
● Use minimal physical restraint
● Seek professional medical assessment as soon as possible
Because naloxone can wear off while opioids remain active, observation for at least several hours in a medical setting is recommended after any overdose. This is particularly important with long-acting opioids like methadone or other opioids with extended duration.
After an overdose: follow-up, treatment and longer-term support
Surviving an overdose is a critical opportunity for you to review opioid use, consider treatment options, and reduce future risk. This should ideally happen with support from drug services as soon as possible after the event.
Typical pathways following overdose:
● Rapid re-engagement with community drug treatment
● Opioid substitution therapy (methadone or buprenorphine)
● Psychosocial interventions and counselling
● Consideration of residential detox or rehabilitation where clinically appropriate
● Each case is assessed on a case by case basis
The risk of further overdose is particularly high in the weeks following discharge from hospital, prison release, or inpatient detox. During these periods, tolerance is reduced, and returning to previous doses can be fatal. Early follow-up and harm-reduction support—including renewed naloxone supply—are absolutely essential!
Family members and significant others often benefit from information, support and training in naloxone use. They are frequently the people most likely to be present at future emergencies.
Organisations like PCP operate residential rehab and detox services within the UK system, working alongside NHS and local services to provide structured treatment, aftercare and relapse-prevention planning for people who choose this route.
Harm-reduction measures like naloxone and safer-use advice can sit alongside aspirations for abstinence or long-term recovery—they are not in opposition to one another. The priority is keeping you alive so you have the opportunity to access other medicines and treatment when ready.
Key Points to Remember
● Naloxone is a temporary opioid antagonist used to reverse life-threatening respiratory depression from opioid overdose
● It is not a cure for addiction and is not a substitute for emergency medical care
● UK legislation from 2015, 2019 and 2024 allows a wide range of services and workers to supply take home naloxone without individual prescriptions for emergency use
● Anyone can administer naloxone in an emergency in the UK to save life
● 999 must always be called in any suspected overdose
● Repeated dosing and close observation may be necessary because naloxone’s effects can wear off while opioids remain active
● If you use opioids, or if you live or work with people who do, you should find out how to obtain naloxone and overdose training from your local NHS, council, or specialist drug and alcohol services
Combining harm-reduction tools like naloxone with access to evidence-based treatment and psychosocial support offers the best chance of reducing overdose deaths and supporting recovery. Whether legal restriction debates continue or wider access develops, the core message remains absolutely clear: carry naloxone if you are at risk of witnessing an overdose, learn how to use it, and always call 999!
For information about accessing naloxone in your area, contact your local drug and alcohol service, community pharmacy, or visit your local NHS or council website. If you or someone you know is struggling with opioid dependence and considering treatment options, services including residential rehabilitation can provide careful consideration of the best pathway forward.
Author
-
View all posts
Andy's journey in psychology and substance recovery is marked by significant educational and professional achievements. He studied Person Centered Counseling, gained insights from psychological literature, and completed an online course on the mind. His hands-on experience includes volunteering at a Drug and Alcohol Clinic and earning a diploma in child adverse experiences. Andy holds a first-class honors degree in Psychology with Substance Use and Misuse. Professionally, he has contributed as a Lived Experience Coordinator and counselor, offering hope and empowerment to those in recovery.
Qualifications and Experience:
Introductory Course in Person Centered Counseling
Extensive study of psychological literature (including Carl Rogers and Freud)
Online course completion on the Mind from UCT
OCN peer mentoring course
Level 3 diploma in child adverse experiences
First-class honors degree in Psychology with Substance Use and Misuse
Experienced Lived Experience Coordinator for Probation Dependency and Recovery service